|
Every climber in Denali should be familiar with both prevention and proper treatment of the most common medical ailments seen on mountaineering expeditions, namely Acute Altitude Sickness (AMS, HACE, HAPE), Frostbite, and Gastrointestinal Illness. The following recommendations were derived from a panel of Wilderness Medical Society experts. 
ACUTE ALTITUDE SICKNESSPrevention
|
| Acute Mountain Sickness (AMS) | |
| Signs/Symptoms | Headache with one or more of the following:
|
| Treatment |
|
| High Altitude Cerebral Edema (HACE) | |
| Signs/Symptoms |
|
| Treatment |
|
| High Altitude Pulmonary Edema (HAPE) |
|
| Signs/Symptoms |
|
| Treatment |
|
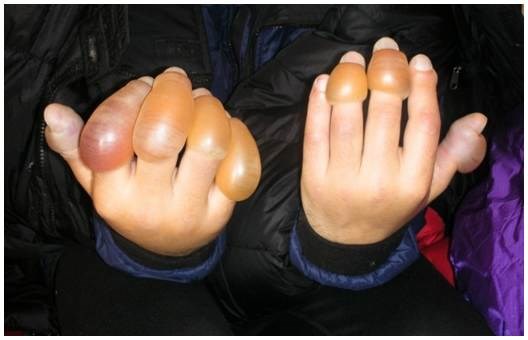
FROSTBITE
Prevention
Maintain peripheral perfusion/circulation
-
Maintain core body temperature
-
Maintain adequate hydration
-
Cover exposed skin
-
Minimize blood flow restriction with constrictive clothing/footwear
-
Do not tolerate numbness -- actively re-warm extremities
Exercise
-
Physical activity elevates core/peripheral temperatures and can be protective against cold injury
Protection from cold
-
Avoiding perspiration as moisture hastens the effects of cold/wind
-
Increase clothing insulation layers
-
Consider chemical hand/foot/core warmers
| Superficial Frostbite (1st and 2nd degree) | |
| Signs/Symptoms |
|
| Treatment |
|
| Deep Frostbite (3rd and 4th degree) | |
| Signs/Symptoms |
|
| Treatment |
|
GASTROINTESTINAL ILLNESS
Gastrointestinal illness is another frequent complaint of expedition climbers throughout the world. The best way to prevent a digestive tract illness is through proper sanitation practices. The National Park Service mountaineering rangers work diligently to maintain a clean mountain environment through education and policy enforcement. Each climber and their team are expected to adhere to the policies outlined on this website and presented at the climber orientations in Talkeetna.
OTHER RECOMMENDED READING
For additional information on these and other mountaineering-related medical issues, see the Mountain Medicine section of our Recommended Reading List.
|
Sources:
|
Last updated: January 31, 2025
